Post-Covid Conditions and the Recovery Process
- Students vs. Pandemics

- Apr 20, 2023
- 4 min read
Written by Amanda Abusaif, Edited by Maura McDonagh, Justin Nguyen, and Courtney Coleman

Onset of COVID-19 can lead to a myriad of different symptoms of varying severity depending on the person, usually fever, fatigue, congestion, and difficulty breathing. However, sometimes symptoms of COVID-19 can continue after recovery from initial infection, even for healthy young adults. When someone experiences a symptom of COVID-19 after four weeks or more after initial recovery from acute COVID-19 onset, this symptom is called a “post-COVID condition.” This could occur following mild or severe COVID-19 infection. In the media, these conditions can also be called long COVID and post-acute COVID-19 syndrome, among other names. Symptoms of COVID-19 infection can range from mild to severe, as can post-COVID conditions. However, the prevalence and severity of “post COVID” are important to consider since they may lead to long-term tissue damage. In a prospective cohort study done in Rome, Italy, 87.4% of 143 patients who had recovered from COVID-19 reported at least one post-COVID condition after an average of 60.3 days since the initial infection. Fatigue and difficulty breathing (dyspnea) were the most commonly-reported post-COVID conditions in this cohort.
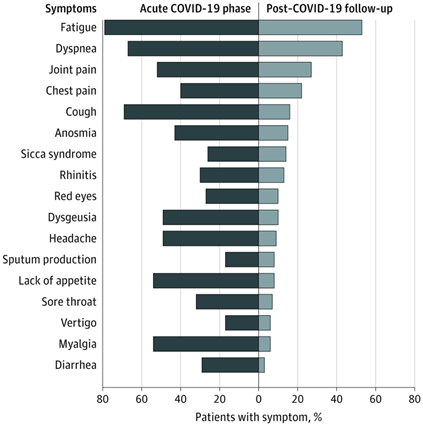
Fig 1 Percentage of patients with COVID-19 symptoms and post conditions. Note how 53.1% of patients reported fatigue during the follow-up visit, and 43.4% reported dyspnea. “Acute” means recent onset of COVID-19 (Carfì et al., 2020).
Post-COVID conditions can be recurring, ongoing, or even new symptoms that arise after recovery from initial infection. Common conditions as a result of the disease damaging organs include:

● Difficulty breathing (dyspnea)
● Fatigue
● Cough
● Chest pain
● Headache
● Irregular heartbeat
● Abdominal pain
● Diarrhea
● Insomnia
● Fever
● Lightheadedness
Fig 2 Common Post-COVID conditions. According to the CDC,
ongoing or new symptoms after initial recovery from COVID-19
include dyspnea, headache, irregular heartbeat, and fever.
COVID-19 infection can damage and inflame the heart, which can lead to long-term abnormal breathing, chest pain, and irregular heartbeat. There can also be post-COVID conditions that are not a direct result of the disease but rather from hospitalization, known as post-intensive care syndrome, which includes symptoms such as weakness, PTSD, and cognitive impairment, manifesting as difficulty with memory and attention.
More research needs to be done on the mechanisms of post-COVID conditions, but it has been found that three months after COVID infection, SARS-CoV-2 RNA can be detected in the upper respiratory tract at lower levels than during infection. SARS-Cov-2 RNA contains the genetic information to replicate the virus after it hijacks the host cell; however, those with the RNA after initial infection showed no or mild symptoms, so it is still unclear if recurrent RNA plays a role in post-COVID conditions. It was found that those with recurrence of SARS-CoV-2 RNA have a low chance of infecting others with COVID-19. The exact cause for this recurrence with lower transmissibility is still not known, but more research is being conducted.
For someone recovering from COVID-19 at home, one should monitor any post-COVID conditions that arise to avoid long-term damage. If you can, it is highly recommended to call your regular primary care provider as soon as possible for proper instructions on how to recover at home that might cater to you better. Try to monitor systems such as temperature, breathing difficulty, fatigue, and chest pain, and to report them to your primary care provider for more instructions. It is also important to rest and stay hydrated. Water, herbal tea, and soups can be helpful, while caffeine and alcohol should be avoided. If you experience a medical emergency (severe difficulty breathing, losing consciousness, dehydration, fever over 102 degrees), call 911, or go to a local hospital immediately. If the situation is not serious, you can call your primary care provider.
It is recommended that people should test for COVID-19 one and two months after initial recovery from acute COVID-19 onset, since about one in ten people test positive for SARS-CoV-2 RNA within 60 days after initial recovery. More research is needed to determine if the recurring SARS-CoV-2 RNA is capable of causing infectious transmission, so as of now, those in the recovery process should be cautious of this transmission possibility.
The best way to avoid post-COVID conditions and long-term consequences of COVID-19 is to avoid contracting COVID-19. Some populations are at higher risk to suffer severe COVID-19 symptoms and post-COVID conditions. The table below summarizes information from the CDC on how higher-risk populations can protect themselves.

There is still much research to be done on post-COVID symptoms and how to recover from them, as this is essential to understand the full impact of COVID-19 on the human body and the recovery process. The elderly, those who are immunocompromised, and pregnant women are more likely to get severely sick from COVID-19 and thus suffer post-COVID conditions. Preventing post-COVID conditions involves preventing COVID-19 infection in the first place by: getting vaccinated, wearing a mask, social distancing, washing hands often, and avoiding crowds.
This post is not a substitute for professional advice. If you believe that you may be experiencing the symptoms of COVID-19, please contact your primary care physician, or go to the nearest Emergency Room. Results from ongoing research and the current understanding of COVID-19 are constantly evolving. This post contains information that was last updated on April 20, 2023.










Comments